You shouldn’t ignore the signs your body’s sending you—irregular periods, stubborn weight gain, unexpected hair growth, and persistent acne can all point to PCOS, a hormonal condition affecting millions of women who deserve answers. If you’re also experiencing hair thinning, pelvic pain, fertility struggles, exhaustion, or mood changes, your body might be trying to tell you something important. Understanding these ten warning signs can be the first step toward getting the care you need.
Key Takeaways
- Irregular or missed periods indicate potential PCOS disrupting ovulation and hormone signals regulating your menstrual cycle.
- Unexplained weight gain around the midsection suggests insulin resistance, a hallmark feature of PCOS affecting fat storage.
- Excess facial and body hair results from elevated androgen levels causing unwanted hair growth patterns.
- Persistent acne resistant to standard treatments stems from hormonal imbalances increasing sebum production on skin.
- Anxiety, depression, and brain fog signal hormonal fluctuations affecting neurotransmitter activity and mental health functioning.
Irregular or Missed Periods

When your cycle’s all over the place—sometimes showing up late, sometimes not at all—it’s one of the most common red flags for PCOS. You might experience periods that stretch weeks apart or skip months entirely, which can feel pretty unsettling if you’re used to regular cycles.
Here’s what’s happening: PCOS disrupts your hormone levels, particularly insulin and androgens, which throw off the signals that trigger ovulation. Without regular ovulation, your uterine lining doesn’t shed on schedule.
This irregularity isn’t just inconvenient—it’s actually your body’s way of telling you something’s off balance. You shouldn’t brush it off as stress or normal variation, especially if the pattern’s been going on for months. Tracking your cycles and noting these changes gives you valuable information to bring to your doctor. It’s genuinely one of the earliest clues that PCOS might be worth investigating.
Weight Gain You Can’t Shake

If you’re eating pretty much the same as you always have but the scale keeps creeping up, PCOS might be the culprit behind that stubborn weight gain.
Here’s what’s happening: PCOS messes with your insulin levels, making your body hold onto fat more aggressively. You’re not imagining things—this isn’t about willpower or calories alone.
PCOS disrupts insulin levels, causing your body to cling to fat more stubbornly—it’s not about willpower alone.
- Insulin resistance makes your body store more fat, especially around your midsection
- Hormonal imbalances slow your metabolism and increase hunger signals
- Difficulty losing weight even when you’re trying harder than ever
- Increased appetite from elevated androgen levels makes restraint feel impossible
The frustrating part? Traditional dieting often doesn’t work the same way for you. Your body’s playing by different rules. Weight management with PCOS requires understanding these hormonal shifts, not just eating less. Many women find success by addressing the underlying insulin resistance through specific dietary approaches and working with healthcare providers who understand PCOS.
Excess Hair Growth in Unexpected Places

You’ve probably noticed extra hair sprouting in places you’d rather it didn’t—your chin, upper lip, or belly—and that’s hirsutism, a direct result of the hormonal imbalance PCOS creates. Understanding where this unwanted hair typically appears and why it happens helps you recognize this common PCOS symptom. We’ll explore the hormonal mechanisms behind hirsutism and discuss the treatment and management options that can help you regain control.
Hirsutism and Hormonal Imbalance
One of the most bothersome signs of PCOS is hirsutism—unwanted hair growth that shows up in places you’d rather it didn’t. You’re dealing with excess androgens, or male hormones, that your body’s overproducing.
This hormonal imbalance triggers hair to sprout on your:
- Face, chin, and upper lip
- Chest and abdomen
- Back and shoulders
- Arms and legs
The frustrating part? You can’t just shave it away permanently. You’re fighting a hormonal issue, not a grooming problem. That’s why tackling PCOS itself matters more than constantly reaching for razors or wax strips. Understanding that hirsutism signals deeper hormonal disruption helps you seek proper treatment and manage your symptoms effectively.
Where Hair Growth Appears
PCOS doesn’t play by the rules when it comes to where hair decides to grow. You might notice dark, coarse hair sprouting on your chin, upper lip, or jawline—places you’d typically expect peach fuzz instead. Your chest, belly, and back can develop unexpected hair growth too, which catches many women off guard.
The frustrating part? This hair growth pattern mirrors what you’d see in men, thanks to elevated androgens coursing through your system. You’ll find yourself reaching for razors, tweezers, or waxing appointments more often than feels fair.
The location matters because it signals your body’s hormone imbalance. These aren’t random stray hairs—they’re a visible sign that your androgen levels are working overtime, pushing your body toward masculine hair distribution patterns.
Treatment and Management Options
While excess hair growth can feel like an unwelcome fixture of PCOS, you’ve got plenty of ways to tackle it.
You don’t have to accept hirsutism as permanent. Here’s what actually works:
- Topical treatments like eflornithine cream slow hair growth directly where you need it
- Hair removal methods including shaving, waxing, and laser therapy give you quick results
- Hormonal birth control addresses the root cause by regulating androgens
- Lifestyle changes like losing weight and managing stress naturally lower hormone levels
You’ll likely find success combining approaches. Start with what feels most manageable, then add strategies as needed. Talk with your doctor about prescription options too—some medications specifically target PCOS-related hair growth. Remember, managing this symptom takes time, but you’ve absolutely got options worth exploring.
Persistent Acne and Oily Skin

If you’re struggling with stubborn breakouts that won’t quit no matter what you try, you’re not alone—and your skincare routine might not be the culprit. PCOS often triggers persistent acne because elevated androgen levels ramp up sebum production in your skin. This excess oil creates an ideal environment for bacteria to thrive, resulting in those frustrating breakouts that resist typical treatments.
You’ll likely notice your skin feels greasier than usual, even shortly after washing. The acne tends to cluster along your jawline and chin rather than scattered across your face. What makes PCOS acne particularly annoying is its resistance to standard over-the-counter products. Your dermatologist might recommend prescription treatments or mention that addressing your PCOS through hormonal management could greatly improve your skin. Don’t get discouraged—tackling the underlying hormonal imbalance often resolves these stubborn skin issues more effectively than any topical solution alone.
Hair Loss and Thinning in Places You Didn’t Expect
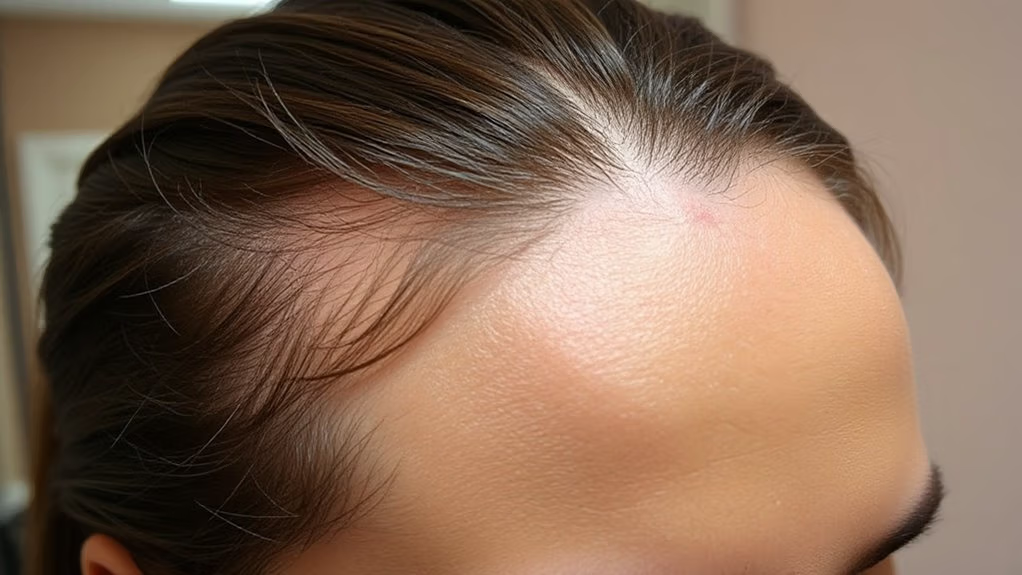
Many women with PCOS notice their hair’s behaving strangely—thinning on top where you’d rather keep it full, while unwanted hair sprouts in unexpected places like your chin, chest, or upper lip.
This frustrating dual effect comes from hormonal imbalance. You’re dealing with excess androgens (male hormones) that shrink hair follicles on your scalp while simultaneously stimulating hair growth elsewhere. It’s like your body’s got its wires crossed.
Here’s what you might experience:
- Noticeable hair loss when you shower or brush
- A receding hairline or widening part
- Coarse, dark facial hair requiring frequent removal
- Unexplained body hair in typically hairless areas
The good news? You’re not losing your mind, and it’s treatable. Once you address the underlying hormonal imbalance through medication, lifestyle changes, or both, your hair can stabilize. Talk to your doctor about options tailored to your situation.
Dark Patches of Skin That Won’t Fade
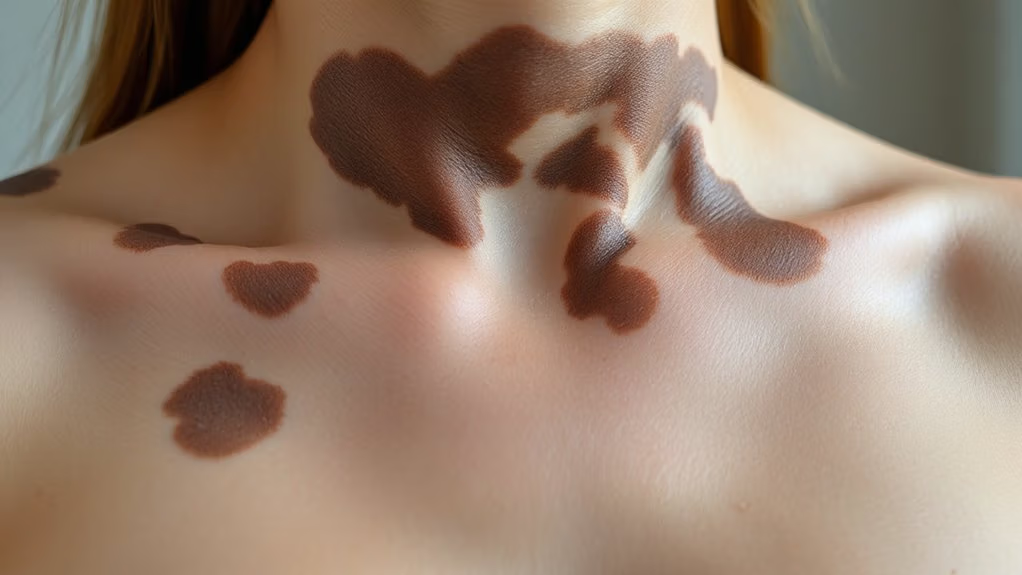
Why does your skin suddenly look darker in random spots, almost like you’ve got permanent dirt you can’t wash off? You’re likely experiencing acanthosis nigricans, a common PCOS symptom triggered by insulin resistance.
| Location | Appearance | Texture |
|---|---|---|
| Neck | Velvety brown patches | Soft, raised |
| Armpits | Dark discoloration | Thickened skin |
| Groin | Shadowy areas | Velvet-like |
| Under breasts | Darkened folds | Slightly rough |
| Knuckles | Hyperpigmented spots | Normal thickness |
These patches develop when your body produces excess insulin, which triggers melanin overproduction in certain areas. They’re not contagious or painful, but they’re definitely bothersome when you’re trying to feel confident.
The good news? They’re reversible. As you manage your PCOS through lifestyle changes, medication, or treatment, these dark patches often fade gradually. Don’t try scrubbing them away—they’ll respond better to addressing the underlying hormonal imbalance. Talk to your doctor about treatment options tailored to your needs.
Pelvic Pain Tied to Your Menstrual Cycle

You might notice that your pelvic pain doesn’t show up randomly—it tends to follow your menstrual cycle pretty closely, and that’s a common experience with PCOS. Understanding what’s triggering your cyclical discomfort can help you anticipate flare-ups and take action before the pain gets intense. When you learn what works best for managing your pain during menstruation, you’ll feel more in control of your body and your month.
Understanding Cyclical Pelvic Discomfort
Pelvic pain that comes and goes with your cycle—sometimes mild cramping, sometimes a nagging ache that won’t quit—is incredibly common with PCOS.
Here’s what you’re experiencing:
- Hormonal surges trigger inflammation in your ovaries and surrounding tissues
- Cyst ruptures can cause sharp, sudden pain during certain cycle phases
- Irregular ovulation means unpredictable pain patterns you can’t quite anticipate
- Prostaglandin buildup intensifies cramping beyond typical period discomfort
You’re not imagining this connection between your cycle and pelvic discomfort. PCOS disrupts your hormone balance, which directly affects how much pain you feel each month. The unpredictability can be frustrating—some months you’re barely aware of anything, other months you’re sidelined.
Tracking when your pain peaks helps you anticipate flare-ups and discuss patterns with your doctor. This information’s valuable for managing your PCOS effectively.
Managing Pain During Menstruation
When menstrual pain’s got you down, there’s plenty you can do to feel better—and you don’t have to white-knuckle your way through every cycle. Start by tracking your discomfort patterns to identify what works best for you.
| Relief Method | When to Use | Effectiveness |
|---|---|---|
| Heat therapy | During cramping | High |
| Over-the-counter NSAIDs | At first sign | High |
| Gentle exercise | Before/during | Moderate |
| Hydration | Throughout cycle | Moderate |
| Prescription medication | Severe pain | Very high |
You’ve got options beyond suffering silently. Anti-inflammatory medications tackle pain at its source, while heat relaxes tense muscles. Movement might seem counterintuitive, but gentle yoga or walking genuinely helps some folks. If over-the-counter solutions aren’t cutting it, chat with your doctor about prescription options designed specifically for menstrual pain management.
Fertility Struggles and Difficulty Conceiving

One of the most heartbreaking signs of PCOS is that it can make getting pregnant much harder than you’d expect. When you’ve got PCOS, your body’s juggling hormonal imbalances that throw off your ovulation cycle, making conception feel like an uphill battle.
PCOS throws your hormonal balance off-kilter, disrupting ovulation and making conception feel like an uphill battle.
Here’s what you might experience:
- Irregular or absent periods that make it nearly impossible to predict your fertile window
- Ovulation that’s sporadic or doesn’t happen at all, leaving you without viable eggs to fertilize
- Higher insulin levels that interfere with the hormones needed for healthy egg development
- Increased androgens that disrupt the delicate balance required for pregnancy
If you’re struggling to conceive after months of trying, don’t brush it off. Many women with PCOS eventually conceive with proper treatment and support. Getting diagnosed early and working with your doctor gives you the best shot at building the family you’re dreaming of.
Exhaustion That Rest Doesn’t Fix

You might notice you’re dragging through your day even after a full night’s sleep, and that’s often connected to PCOS’s hormonal imbalances that disrupt your energy production. Your insulin resistance compounds the problem by making it harder for your body to convert food into usable energy, leaving you perpetually drained. This exhaustion isn’t laziness—it’s your body struggling against metabolic dysfunction that rest alone can’t fix.
Hormonal Imbalances And Fatigue
Because your hormones regulate everything from energy production to sleep quality, PCOS can leave you feeling bone-tired no matter how much you sleep.
When your body’s got too much insulin and androgens floating around, they mess with your metabolism and disrupt your sleep cycles. You’re not being lazy—you’re genuinely exhausted at the cellular level.
What you might notice:
- Waking up feeling like you haven’t slept at all
- Afternoon crashes that hit hard and fast
- Brain fog that makes concentration nearly impossible
- Needing caffeine just to function normally
This fatigue is real and persistent because PCOS throws your endocrine system out of whack. Your body’s working overtime to manage these hormonal fluctuations, draining your energy reserves. Understanding this connection helps you recognize that rest alone won’t fix it—you need proper treatment.
Insulin Resistance Energy Drain
The hormonal chaos we’ve just talked about? It’s directly tied to insulin resistance, which drains your energy in ways that sleep can’t fix.
When your body can’t use insulin efficiently, your cells don’t get the glucose they need for fuel. You’re running on empty even after eight hours of sleep. You might feel wired yet exhausted—that frustrating combination where your body’s exhausted but your mind won’t settle.
| Energy Symptom | What’s Happening | Why It’s Stubborn |
|---|---|---|
| Afternoon crashes | Blood sugar dips rapidly | Insulin dysfunction continues |
| Unrefreshing sleep | Hormones disrupt rest quality | PCOS persists overnight |
| Brain fog | Glucose can’t reach your brain | Cells resist insulin signals |
| Persistent fatigue | Mitochondria underperform | Energy production stays compromised |
This exhaustion isn’t laziness—it’s your metabolism struggling against insulin resistance.
Mood Changes, Anxiety, and Depression

While hormonal imbalances wreak havoc on your body, they’re also wreaking havoc on your mind. PCOS doesn’t just affect your physical health—it impacts your mental wellbeing in real, tangible ways.
The hormone fluctuations you’re experiencing can trigger:
- Persistent anxiety that leaves you feeling on edge throughout your day
- Depression that makes even simple tasks feel overwhelming
- Mood swings that confuse both you and those around you
- Brain fog that makes concentration nearly impossible
You might notice you’re snapping at loved ones more often or feeling overwhelmed by situations you’d normally handle fine. You’re not losing it—your hormones are genuinely affecting your neurotransmitters. This is especially true if you’re dealing with elevated androgen levels, which directly influence serotonin production.
Don’t brush off these mental health changes as just stress or character flaws. They’re legitimate PCOS symptoms deserving professional attention and support.
Conclusion
You’re exhausted yet wide awake with worry. You’re gaining weight while eating right. Your body’s betraying you—hair sprouting where it shouldn’t, vanishing where it should. But here’s the thing: you’re not broken. These aren’t character flaws; they’re your body sending signals you deserve to hear. Talk to your doctor. Get tested. You’ve got this, and you don’t have to figure it out alone.








