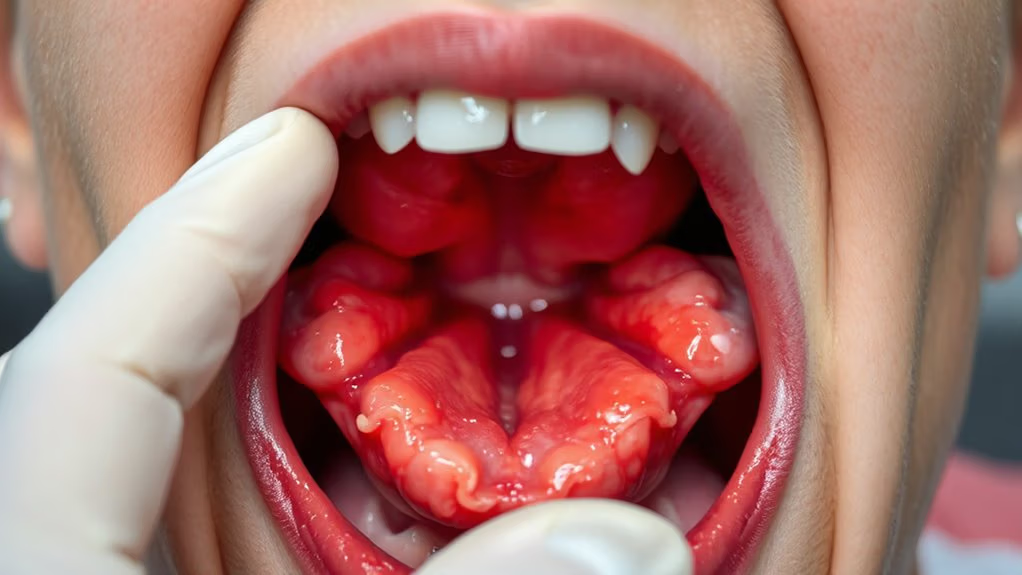
You shouldn’t ignore your gut’s warning signals—they’re telling you something important. If you’re experiencing persistent diarrhea, severe cramping, unexplained weight loss, or bloody stools, it’s time to talk with your doctor. Add in chronic fatigue, canker sores, and recurring fevers, and you’ve got seven red flags that demand attention. These symptoms can sneak up on you, but catching them early makes managing Crohn’s disease so much easier. There’s plenty more to understand about each of these signs.
Key Takeaways
- Persistent diarrhea with urgent bowel movements lasting weeks signals chronic inflammation requiring medical consultation.
- Severe abdominal pain, cramping, and bloody stools indicate intestinal lining damage demanding immediate medical attention.
- Unexplained weight loss and appetite loss reflect poor nutrient absorption characteristic of Crohn’s disease.
- Chronic fatigue persisting despite adequate sleep stems from immune system fighting gut inflammation.
- Canker sores, skin rashes, and fever indicate systemic inflammation requiring healthcare provider evaluation.
Persistent Diarrhea and Urgent Bowel Movements

When you’re making frequent trips to the bathroom and you can’t quite predict when nature’s going to call, that’s a red flag worth paying attention to. Persistent diarrhea isn’t just inconvenient—it’s your body’s way of signaling something’s off.
Frequent bathroom trips and unpredictable urges are red flags your body’s signaling something needs attention.
With Crohn’s disease, you’ll likely experience urgent bowel movements that catch you off guard. You might find yourself running to the bathroom multiple times daily, sometimes without warning. This urgency can disrupt your work, social life, and sleep.
What makes this different from occasional stomach troubles is the consistency. You’re not dealing with a one-time bug; these symptoms stick around for weeks or longer. The diarrhea might be accompanied by blood or mucus, which shouldn’t be ignored either.
If you’re noticing this pattern, don’t brush it off as stress or diet. It’s worth discussing with your doctor, who can help identify whether Crohn’s disease or another condition’s responsible.
Severe Abdominal Pain and Cramping

You’ll notice that Crohn’s pain doesn’t follow a simple pattern—sometimes it’s sharp and localized, other times it’s a dull ache that spreads across your abdomen. The inflammation in your digestive tract is what’s actually behind that discomfort, as your body’s immune system attacks the lining of your gut. If you’re experiencing pain that’s getting worse, doesn’t ease up with over-the-counter meds, or comes with fever or bloody stools, that’s your cue to contact your doctor right away.
Distinguishing Pain Patterns
Abdominal pain’s a tricky thing with Crohn’s disease—it doesn’t always announce itself the same way twice. You might wake up with a dull ache that gradually intensifies, or you could get blindsided by sharp, stabbing sensations. Some days the cramping feels like your insides are wringing themselves out; other days it’s more of a constant, nagging discomfort.
Pay attention to when your pain strikes. Does it flare after eating certain foods? Does it come in waves or stay put? Notice whether it’s localized to one spot or spreads across your abdomen. These details matter because they help you identify your personal pain patterns.
When you can distinguish between your typical cramping and something genuinely different, you’ll recognize when it’s time to call your doctor.
Inflammation’s Role in Discomfort
Because your gut’s inflamed during a Crohn’s flare, that’s where the real trouble starts. Your intestinal lining swells up something fierce, and that inflammation triggers intense cramping and pain you can’t ignore.
Here’s what happens in your body:
| Inflammation Stage | What You Feel |
|---|---|
| Early swelling | Dull, persistent ache |
| Increased inflammation | Sharp, stabbing cramps |
| Severe flare | Debilitating pain that stops you cold |
| Muscle tension | Rigid, board-like abdomen |
| Peak inflammation | Pain radiating through your entire gut |
When inflammation spreads deeper into your intestinal walls, you’re looking at serious discomfort that disrupts your entire day. You might double over, unable to work or leave home. This isn’t just stomach upset—it’s your body signaling real damage happening inside.
When Symptoms Demand Attention
When sharp, unbearable pain grips your belly and won’t let go, that’s your sign to take action—fast. You shouldn’t dismiss severe abdominal pain as something you’ll ride out—it’s your body’s way of demanding help.
If you’re doubled over, can’t eat, or the cramping’s so intense you can’t function, call your doctor immediately. Don’t wait it out hoping it’ll pass. Severe pain combined with other symptoms like fever, bloody stools, or persistent vomiting needs urgent attention.
Your gut’s trying to tell you something’s seriously wrong. Trust that instinct. Severe symptoms can indicate complications like blockages or infections that require prompt medical intervention. Getting checked out quickly protects your health and prevents things from worsening.
Unexplained Weight Loss and Loss of Appetite

You might notice your clothes fitting differently or your belt needing to tighten up a notch, and at first, you’ll think it’s just a good thing—until you realize you haven’t been trying to lose weight.
When Crohn’s disease flares up, your body can’t absorb nutrients properly, leading to unintended weight loss. You’ll find yourself feeling less hungry than usual, even when you know you should eat. Food might seem unappealing, or you’re worried about how it’ll make you feel afterward.
This combination of appetite loss and weight loss is a red flag worth taking seriously. Your body needs fuel to function, and sustained weight loss weakens your immune system further. If you’re dropping pounds without explanation or struggling to eat normally, don’t brush it off. Talk to your doctor about what’s happening. These changes often signal that your Crohn’s needs better management or adjustment to your treatment plan.
Blood or Mucus in Your Stool

Finding blood or mucus in your stool can be alarming, but it’s actually one of the more telling signs that Crohn’s disease is affecting your digestive tract. When your intestines are inflamed, they can’t function properly, and you’ll notice changes in what you’re passing.
| Sign | What It Means |
|---|---|
| Bright red blood | Bleeding closer to the rectum |
| Dark, tarry stool | Bleeding higher in the intestines |
| Visible mucus | Intestinal lining inflammation |
| Frequent urgency | Severe inflammation present |
| Consistency changes | Digestive tract distress |
You shouldn’t ignore these symptoms. Blood in your stool indicates your intestinal lining is damaged and bleeding. Mucus appears when your gut’s trying to protect itself from inflammation. Both warrant immediate attention from your doctor, who can determine severity and adjust your treatment plan accordingly. Don’t feel embarrassed bringing this up—it’s essential information for proper diagnosis.
Chronic Fatigue and Weakness

You might notice that you’re dragging through your day even after a full night’s sleep—that’s inflammatory fatigue talking, and it’s one of Crohn’s sneakier symptoms that can make everything from work to simple household tasks feel exhausting. This relentless tiredness doesn’t just wear you down physically; it can derail your plans, mess with your mood, and leave you wondering why you can’t keep up like you used to. We’ll walk through what’s causing this fatigue and share some practical energy management tactics that can help you reclaim your day.
Understanding Inflammatory Fatigue
When Crohn’s disease flares up, it doesn’t just affect your digestive system—it can leave you feeling absolutely drained, even after a good night’s sleep. This isn’t ordinary tiredness you can shake off with coffee. You’re experiencing inflammatory fatigue, where your body’s immune system works overtime fighting inflammation in your gut, sapping your energy reserves completely.
| Fatigue Type | Cause | Duration |
|---|---|---|
| Inflammatory | Immune response to gut inflammation | During flares |
| Nutritional | Poor nutrient absorption | Ongoing |
| Medication-related | Side effects from treatments | Variable |
| Sleep-disrupted | Nighttime symptoms and pain | During flares |
| Anemia-induced | Low iron from bleeding | Persistent |
Your body’s battling internal inflammation while simultaneously struggling to absorb nutrients properly. You might find yourself canceling plans or struggling through your workday. That heaviness you’re feeling? It’s your signal that something’s brewing inside, and you shouldn’t dismiss it.
Impact On Daily Activities
Because inflammatory fatigue doesn’t respect your schedule or ambitions, it’ll reshape how you move through each day. You might find yourself struggling with tasks you’d previously tackle without thinking twice.
Your body’s sending signals that’ll force you to reconsider what’s realistic:
- Simple errands like grocery shopping or laundry become exhausting expeditions requiring recovery time
- Work productivity suffers when you’re battling brain fog and physical depletion
- Social plans get canceled because you’ve depleted your energy reserves
You’re not being lazy—your immune system’s working overtime, draining resources your body desperately needs. The weakness isn’t something you can push through with willpower alone. You’ll need to listen to what your body’s telling you and adjust expectations accordingly.
Energy Management Strategies
Rather than fight against your body’s limitations, it’s time to work with them. You’ll find that pacing yourself throughout the day makes a real difference. Break tasks into smaller chunks instead of pushing yourself to exhaustion. Listen to your body’s signals—when fatigue hits, rest without guilt.
Prioritize what matters most. Maybe you can’t do everything, but you can tackle your essentials. Consider which activities drain you most and schedule those when your energy peaks, usually mornings for many people.
Don’t underestimate gentle movement like short walks or stretching. They can actually boost energy rather than deplete it. Stay hydrated and eat regular meals to maintain stable blood sugar.
Talk with your doctor about your fatigue patterns. They might suggest adjustments to your treatment plan.
Canker Sores and Skin Rashes
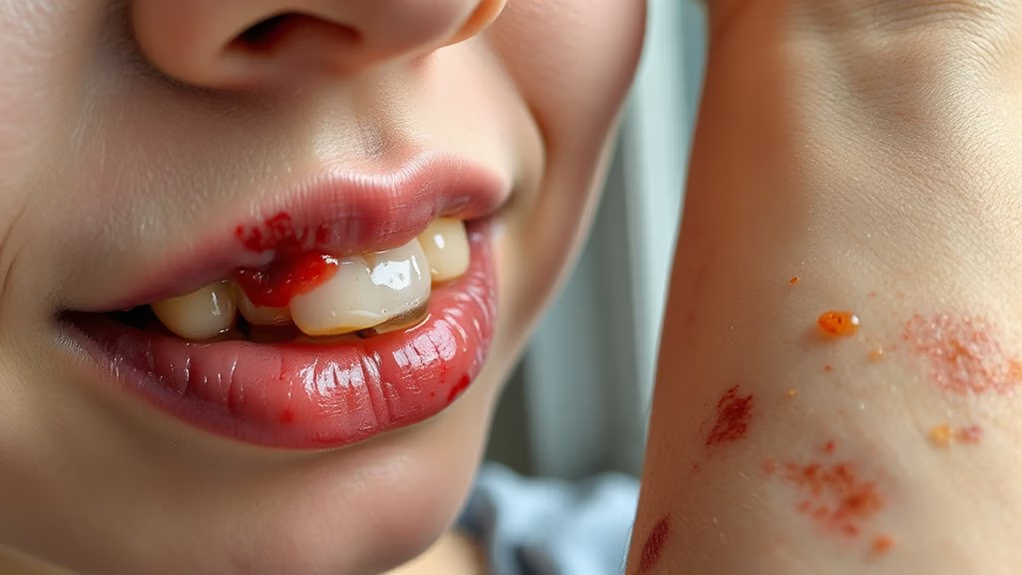
While you’re dealing with digestive troubles from Crohn’s disease, your mouth and skin might be sending distress signals too.
While managing Crohn’s disease, pay attention to distress signals from your mouth and skin—they often reveal systemic inflammation.
Canker sores pop up inside your mouth and can make eating painful. They’re not just annoying—they’re often linked to nutritional deficiencies from poor absorption. You’ll notice small ulcers that sting when you eat or drink.
Skin rashes are another common companion. You might develop:
- Erythema nodosum: tender, red bumps on your shins and forearms
- Pyoderma gangrenosum: painful open sores that need medical attention
- General inflammation: itching and irritation across affected areas
These symptoms aren’t separate from your Crohn’s—they’re your body’s way of flagging systemic inflammation. When you spot canker sores that won’t heal or unusual rashes appearing, don’t brush them off. Report them to your doctor immediately. Catching these warning signs early helps you adjust your treatment plan and prevent complications. Your skin and mouth deserve the same attention as your gut.
Recurring Fever and When to Seek Immediate Care

If you’re running a fever that keeps coming back, your body’s telling you something important. With Crohn’s disease, recurring fevers often signal inflammation flaring up in your digestive tract or an infection developing.
Pay attention to the pattern. A fever that spikes repeatedly over days or weeks deserves medical attention. Track your temperature and note what else is happening—increased pain, diarrhea, or fatigue alongside fever means you shouldn’t wait.
Seek immediate care if you’re experiencing a fever above 103°F, severe abdominal pain, or signs of sepsis like confusion or rapid heartbeat. Don’t hesitate to call your doctor if fever persists beyond three days or worsens despite treatment.
Your gut’s inflammation can lead to serious complications, so trust your instincts. When something feels off, it probably is. Getting prompt medical evaluation helps prevent complications and gets you relief faster.
Conclusion
You’re holding a candle through a foggy forest—these seven warning signs are your light. Your body’s whispering before it shouts. Don’t ignore the rumbles, the aches, the exhaustion creeping in like shadows at dusk. You know yourself best. If your gut’s sending distress signals, reach out to your doctor. Trust what you’re feeling. Getting answers isn’t weakness; it’s wisdom.