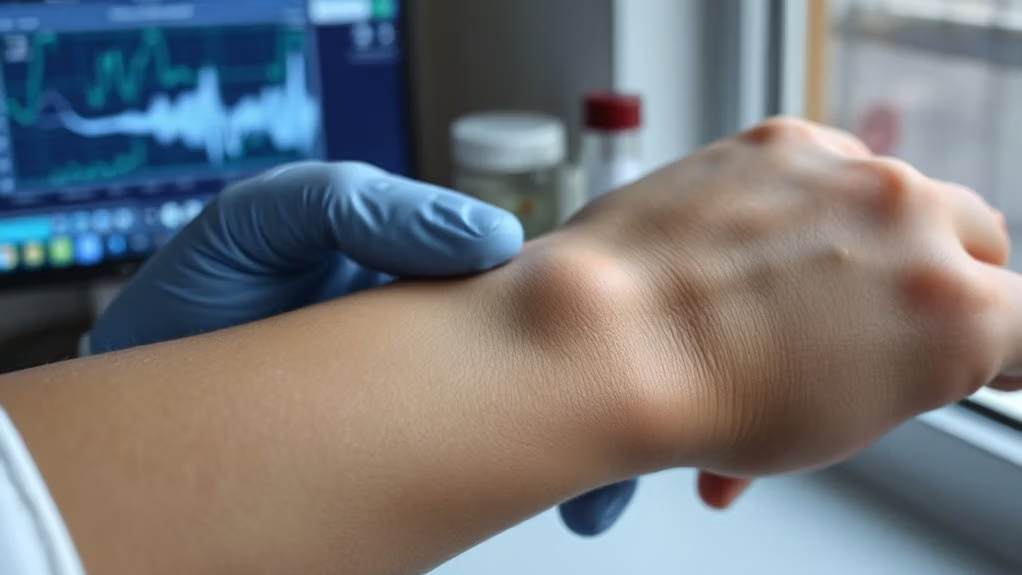
You’re probably brushing off those creaky joints and morning stiffness as just getting older, but they’re your body’s first alarm bells. You might notice your hands feel stiff when you wake up, joints look puffy or feel warm, and you’re losing your grip strength on simple tasks like opening jars. Add in that bone-deep exhaustion that won’t quit, even after rest, and you’ve got real warning signs. Your doctor needs to hear about this—especially if swelling sticks around or stiffness lasts past thirty minutes. Understanding what’s really happening inside your joints reveals why timing matters so much.
Key Takeaways
- Creaky, stiff joints that improve with movement but return after inactivity signal early arthritis.
- Morning stiffness lasting hours and difficulty gripping objects like coffee cups indicate joint inflammation.
- Puffy, warm joints with symmetric swelling across both sides suggest inflammatory arthritis development.
- Unexplained fatigue resistant to rest, especially accompanying joint pain, warrants medical evaluation.
- Persistent swelling, morning stiffness beyond 30 minutes, and warmth around joints require doctor attention.
Joint Pain and Stiffness: The First Warning Signs

Creaky joints—they’re often what bring folks to the doctor’s office first. You might notice your knees feel stiff when you climb out of bed in the morning, or your fingers don’t bend quite as smoothly when you’re making your morning coffee.
These early warning signs matter because they’re your body’s way of telling you something’s shifting. You may experience mild discomfort that comes and goes, or persistent aching in your hands, knees, hips, or shoulders. The stiffness typically improves once you get moving, but it might return after you’ve sat still for a while.
Pay attention if you’re reaching for pain relievers more frequently or if these sensations last longer than a few weeks. You shouldn’t ignore these signals—they’re often arthritis’s quiet introduction. Getting checked early means you can take steps to slow progression and keep doing what you love.
Morning Stiffness That Lasts Hours

You’ll notice that your morning stiffness doesn’t just fade in a few minutes—it’s the kind that lingers for hours, making those first movements feel like you’re moving through molasses. The severity can swing wildly day to day, and understanding these patterns helps you figure out what’s really going on with your joints. Learning the right stretching techniques gives you real relief and helps you reclaim those stiff mornings.
Duration And Severity Patterns
When arthritis sets in, one of the telltale signs that something’s amiss is how your joints rebel first thing in the morning. You’ll notice patterns emerging—some mornings feel worse than others, and the stiffness doesn’t budge for hours.
| Time of Day | Stiffness Level | Duration | Activity Impact | Relief Method |
|---|---|---|---|---|
| Upon waking | Severe | 1-2 hours | Can’t grip coffee cup | Warm shower |
| Mid-morning | Moderate | 30-60 minutes | Stiff movements | Light stretching |
| Afternoon | Mild | 15-30 minutes | Nearly normal | Continued activity |
| Evening | Variable | 1-3 hours | Fatigue sets in | Rest and heat |
| Night | Increases | Throughout sleep | Affects sleep quality | Compression wraps |
Pay attention to these patterns. They’re your body’s way of communicating what’s happening beneath the surface.
Stretching Techniques For Relief
Now that you’ve spotted the pattern—that brutal morning stiffness that won’t quit—it’s time to fight back with some simple stretches that’ll get your joints moving again.
Start gentle. Before you even climb outta bed, try slow ankle circles and gentle knee bends. Once you’re upright, reach toward your toes—don’t force it, just breathe into the stretch. Hold each one for thirty seconds.
Neck rolls work wonders too. Slowly rotate your head in circles, loosening that tension that’s built up overnight.
The key’s consistency. You’ve gotta stretch every morning, not just when the pain’s screaming loud. Think of it like oiling a rusty hinge—regular maintenance keeps things moving smoother than waiting until everything’s completely seized up.
Swelling, Warmth, and Visible Changes Around Joints

You might notice your joints looking puffy or feeling warm to the touch—signs that shouldn’t be ignored. These changes often come with redness around the affected area, making it hard to miss what’s happening in your body. If you’re spotting visible deformities or your joints feel hot even when you’re resting, it’s time to talk with your doctor about what’s going on.
Joint Swelling and Puffiness
One of arthritis’s telltale signs shows up right before your eyes—your joints start looking puffy and feel warm to the touch. You’ll notice your knuckles, wrists, or knees appear swollen, like someone’s turned up the volume on inflammation. That puffiness? It’s fluid buildup from your immune system attacking joint tissues. Your fingers might feel tight when you make a fist, or your shoes could suddenly feel snug around the ankles. The warmth accompanying this swelling hints at active inflammation happening beneath the skin. These changes often appear symmetrically—affecting the same joints on both sides of your body. If you’re spotting this pattern regularly, especially alongside stiffness that lingers after rest, it’s worth discussing with your doctor sooner rather than later.
Heat and Warmth Sensation
When inflammation kicks into high gear, your joints don’t just swell—they practically radiate heat like they’re running a fever of their own. You’ll notice warmth radiating from your knees, hands, or shoulders, sometimes even before visible swelling appears. This heat sensation comes from increased blood flow to the inflamed area as your body mounts its immune response.
That warmth you’re feeling? It’s your joints’ way of waving a red flag. You might touch your joint and feel it’s noticeably warmer than surrounding skin. This symptom often accompanies stiffness and tenderness, creating a trifecta of discomfort. Pay attention when you notice this persistent warmth, especially if it lingers beyond a few days or spreads to multiple joints. These heat signals deserve medical attention.
Visible Deformities and Changes
As arthritis progresses, your joints don’t keep their secrets—they start showing their damage in ways that’re hard to miss. You’ll notice your knuckles or knees swell up, sometimes overnight. That puffiness isn’t just uncomfortable; it’s your body waving a red flag.
Your joints might feel warm to the touch, almost feverish around the affected area. The skin overlying them can turn slightly red or take on a shiny appearance. These visible changes often accompany that heat sensation you’ve been experiencing.
Over time, you might see actual deformities develop. Your fingers could start bending at odd angles, or your joints may shift noticeably out of alignment. These changes don’t happen instantly, but once you spot them, you’ll know something’s seriously off with your joints.
Loss of Grip Strength and Hand Mobility

You’ve probably noticed it without really thinking much about it—that jar that used to open with a quick twist now requires both hands and a grunt of effort.
This sneaky loss of grip strength often signals early arthritis. Your hands contain numerous small joints that inflammation targets first, making even simple tasks feel surprisingly difficult. You might struggle opening bottles, turning doorknobs, or holding utensils comfortably during meals.
Beyond strength, you’re likely experiencing reduced hand mobility. Your fingers feel stiff, especially after resting, and movements that once felt automatic now require conscious effort. You might notice swelling across your knuckles or feel a slight burning sensation.
These changes frequently appear before visible deformities develop, making them essential early warning signs. If you’re experiencing consistent grip weakness or mobility challenges, it’s worth discussing with your doctor. Early intervention can make a meaningful difference in managing arthritis progression.
Unusual Tiredness That Won’t Go Away

Many people chalk it up to a busy schedule, but there’s a particular kind of exhaustion that comes with early arthritis—one that doesn’t budge no matter how much sleep you get. This fatigue stems from your body’s inflammatory response working overtime, draining your energy reserves in ways rest alone can’t fix.
You might notice you’re wiped out after light activities that never bothered you before. That’s your body fighting inflammation 24/7. Here’s what often accompanies this tiredness:
- Afternoon crashes that hit like a wall
- Difficulty concentrating or “brain fog”
- Waking up already feeling exhausted
- Needing more sleep yet still feeling drained
If you’re experiencing persistent fatigue alongside joint stiffness or pain, don’t dismiss it as merely needing more rest. Your body’s sending signals worth listening to. Chat with your doctor about what you’re experiencing—early intervention can make a real difference in how you feel moving forward.
How to Tell If It’s Rheumatoid Arthritis vs. Osteoarthritis
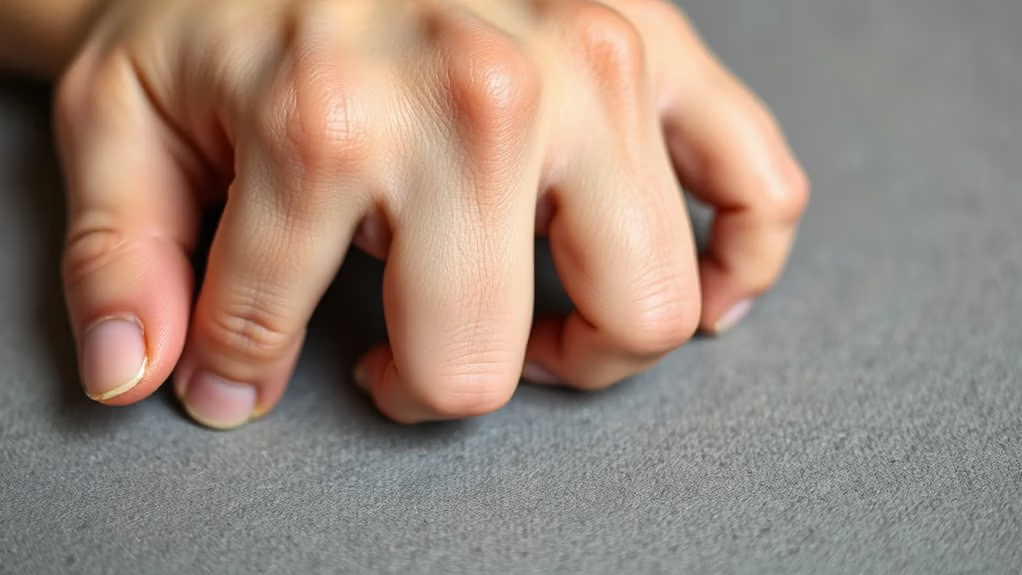
When joint pain shows up, figuring out whether you’re dealing with rheumatoid arthritis (RA) or osteoarthritis (OA) isn’t just academic—it changes everything about how you’ll manage it.
Here’s the real difference: OA’s wear-and-tear damage typically hits your weight-bearing joints—knees, hips, lower back. You’ll notice stiffness that loosens up after you move around. RA, though, plays by different rules. It’s an autoimmune condition that attacks multiple joints symmetrically, so both your hands might swell simultaneously. You’ll feel that stubborn fatigue we mentioned earlier, plus morning stiffness that can last hours.
RA often strikes younger folks and comes with systemic symptoms like fever or general malaise. OA creeps up gradually, usually after fifty. Only blood tests can definitively confirm RA—your doctor looks for specific antibodies—but knowing these distinctions helps you recognize what’s happening in your body.
Red Flags That Demand a Doctor’s Appointment

Sure, some joint aches are just part of life, but certain warning signs shouldn’t be ignored—they’re your body’s way of telling you it’s time to get professional eyes on what’s happening. You’ve got to pay attention when symptoms shift into concerning territory.
Here’s what should send you straight to your doctor:
- Persistent swelling that doesn’t improve after a few days of rest
- Morning stiffness lasting more than 30 minutes, making it tough to start your day
- Unexplained fatigue alongside joint pain, suggesting systemic inflammation
- Warmth or redness around your joints, indicating active inflammation
Don’t brush these off as normal aging. Your joints’re communicating something important. Early intervention makes a real difference in managing arthritis effectively. Trust your instincts—if something feels off, it probably is.
What Happens at Your First Rheumatology Visit
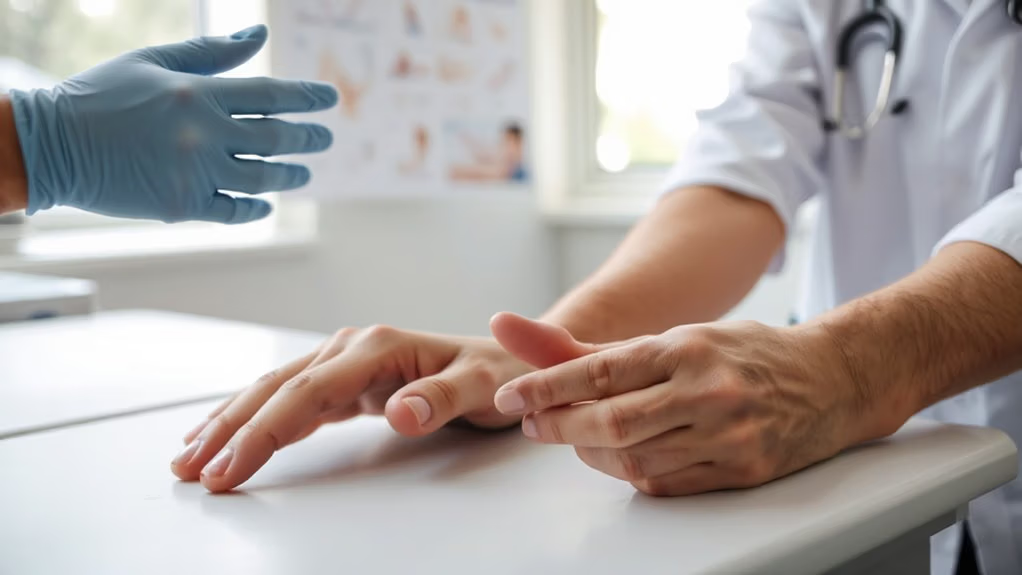
Your rheumatologist will start by asking you about your medical history and when your symptoms first showed up, getting the real story of what’s been going on with your joints. Then comes the hands-on part—they’ll examine you, run some blood tests and maybe take X-rays to see what’s actually happening under the surface. From there, they’ll work with you to build a treatment plan that fits your life and gets you feeling better.
Medical History and Symptoms
The first visit to a rheumatologist isn’t unlike visiting any other doctor, except this time you’re walking in because something’s been bothering you—maybe your knuckles ache after you’ve been typing, or you can’t quite grip a jar like you used to. Your rheumatologist will dig into your story, asking detailed questions about what you’re experiencing:
- When did your symptoms start?
- Which joints hurt, and does the pain move around?
- Does morning stiffness slow you down?
- What makes it better or worse?
They’ll also ask about your family history, lifestyle, and any previous injuries. This conversation matters because arthritis wears different masks. Your honest answers help them piece together whether you’re dealing with osteoarthritis, rheumatoid arthritis, or something else entirely.
Physical Examination and Testing
Once your rheumatologist‘s got the full picture of what you’ve been experiencing, they’ll put down their pen and get hands-on. They’re gonna check your joints—pressing, bending, and watching how you move. They’ll note any swelling, warmth, or tenderness that shows up.
Then come the tests. You’ll likely get blood work to spot inflammatory markers like rheumatoid factor or anti-CCP antibodies. X-rays might follow, revealing bone changes or cartilage damage. Sometimes they’ll order an ultrasound or MRI for a closer look at what’s happening inside.
Don’t worry if results seem confusing at first. Your rheumatologist will walk you through everything, connecting the dots between your symptoms, physical findings, and test results to nail down what’s really going on.
Treatment Plan Development
After all that poking, prodding, and testing, here’s where it gets real—your rheumatologist won’t just hand you a diagnosis and send you on your way. They’ll craft a personalized roadmap tailored to your specific situation. Your treatment plan considers:
- Your arthritis type and severity
- Lifestyle factors and work demands
- Other health conditions you’re managing
- Your goals and preferences
Your rheumatologist explains medication options, from anti-inflammatories to biologics, discussing potential side effects honestly. They’ll talk physical therapy, exercise modifications, and whether you need specialist referrals. You’ll schedule follow-up appointments to monitor progress and adjust treatments as needed. They’re not just treating inflammation—they’re helping you reclaim your life, one strategic decision at a time.
Why Starting Treatment Now Prevents Long-Term Damage

catching arthritis early is like stopping a small leak before it floods your whole house.
When you start treatment now, you’re literally changing your future. Early intervention slows joint damage, preserves your mobility, and keeps you doing what you love longer. You’re not just managing pain—you’re protecting cartilage and bone from irreversible harm.
| Timeline | Without Treatment | With Early Treatment | Your Outcome |
|---|---|---|---|
| Year 1 | Damage accelerates | Inflammation controlled | You stay active |
| Year 5 | Significant deterioration | Minimal progression | Better quality of life |
| Year 10 | Severe limitation | Manageable condition | Independence preserved |
| Year 20 | Potential disability | Sustained function | Years of normalcy |
Think of it this way: you wouldn’t ignore rust on your truck. Your joints deserve the same attention. Starting treatment now means you’re investing in yourself—fewer surgeries, less medication down the road, and a life that doesn’t revolve around pain.
Next Steps: Building Your Arthritis Management Plan

Now that you’ve decided to take action, it’s time to build a plan that actually works for your life. Think of it like mapping out a road trip—you wouldn’t just start driving without knowing where you’re headed.
Your arthritis management plan should include:
- Regular doctor visits to track your progress and adjust treatments as needed
- Daily movement routines that keep your joints flexible without overdoing it
- Pain management strategies combining medication, ice, heat, and rest periods
- Lifestyle tweaks like modifying activities and using assistive tools
Start small. Maybe you’ll begin physical therapy this week and tackle dietary changes next month. Don’t expect perfection overnight—arthritis management’s a marathon, not a sprint. Work closely with your healthcare team, stay consistent, and listen to your body. You’ve got this.
Conclusion
You’ve got to listen when your joints start whispering their complaints—those early signs aren’t just noise, they’re your body’s way of asking for help. Don’t put off that doctor’s visit; catching arthritis early is like stopping a leak before it floods the whole house. You’re the captain of your own ship here, and getting treatment now means you’ll keep sailing smooth for years to come. Your future self will thank you for taking action today.